News and reports
Latest news and views

Have Your Say: Share Your Experience of GP Services in Cornwall
🩺 Have you recently contacted your GP practice? Was it easy to get help? Did you feel heard and supported? Were you happy with the care you received?
We want to know what it’s really like for people across Cornwall when accessing GP…
We want to know what it’s really like for people across Cornwall when accessing GP…
News
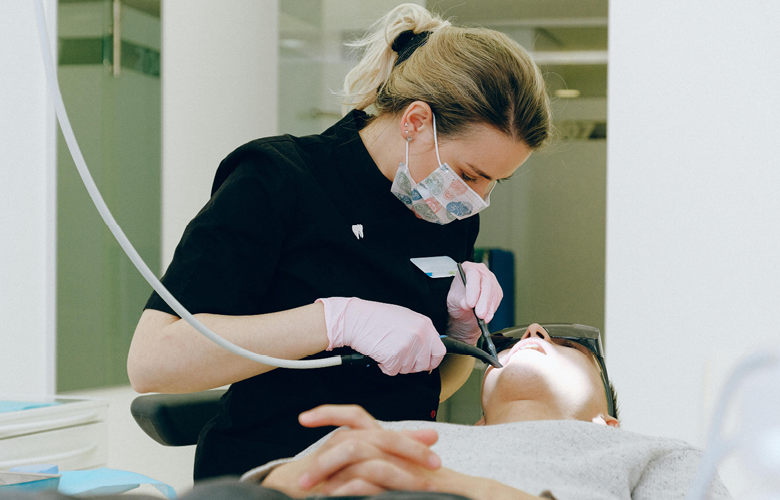
Help Shape the Future of Dental Care in Cornwall – Share Your Experience!
At Healthwatch Cornwall, dental care is the top issue that residents have consistently brought to our attention. In 2023, 36% of all feedback we received was about challenges accessing dental services, and this trend continues into 2024. We want to dig…
News

Mental Health Partnership Board, 17 July 2025
Join our Mental Health Partnership Board and make a real impact on mental health services in our community
News

Don’t destroy our independent voice
Last Friday, Ministers revealed plans to abolish Healthwatch England.
News

Carers Partnership Board, 10 July 2025
Join us on 10th July 2025 for the Carers Partnership Board meeting at Truro Library!
News
Latest reports and publication

Camborne Redruth Community Hospital Minor Injuries Unit Enter and View Report
Healthwatch Cornwall champions better standards of care in socially funded health and social care services.
Find out more

Camborne Redruth Community Hospital Wound Clinic Enter and View Report
Healthwatch Cornwall champions better standards of care in socially funded health and social care services.
Find out more